Today’s guest post is from Emily Wax, an RD from Brooklyn and the blogger behind Eating Chalk. Emily and I have actually gotten to meet in person! I love that she loves sardines like me. Having just gone through a pregnancy (ok, wow, it was actually almost two years ago!), I loved reading her post. Hope you will too!
![]()

Hi, Kath Eats readers! I’m Emily, a Registered Dietitian from NYC who works primarily in outpatient women’s health with prenatal patients. I’ve spent a lot of time thinking about exactly what moms-to-be need to know about nutrition. It can be a pretty involved topic and your specific needs and recommendations will depend on a myriad of factors that should be discussed with your OB-GYN and one-on-on with a RD. For this post, I will stick with some of the basics of nutrition for a healthy pregnancy. I will not be addressing anemia, preeclampsia, gestational diabetes, or multiple gestations, but please feel free to ask questions that go beyond this post in the comments.
A Weighty Topic
Weight gain is an inevitable part of all pregnancies. If you’ve been in weight loss mode this can be a hard switch mentally, so it is helpful to picture exactly where the weight is going.

The Institute of Medicine weight gain recommendations for single fetus pregnancies are based on pregnancy body mass index (BMI), as recommended by the World Health Organization.
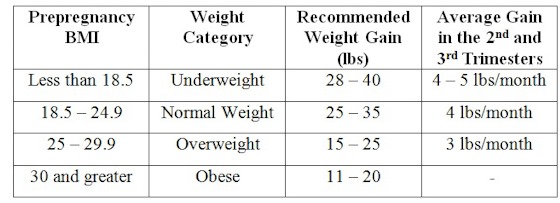
While each patient is treated on a case-by-case basis, you’ll notice that the general recommendation is always to gain weight, even for women who are obese before they get pregnant. Remember that BMI is not an appropriate metric to use during pregnancy once weight gain has begun.
Common Myths
Can you think of any condition other than pregnancy that causes perfect strangers to think it’s acceptable to rub another adult’s belly? Our society has a nasty habit of attempting to assert personal beliefs on women’s bodies. Note to the general public – if you are not part of the medical team and you were not part of the conception, your opinion probably isn’t necessary.
There are too many old wives’ tales concerning pregnancy to list here; I’ve heard everything from “my mom says I can’t have pineapple or hot sauce” to “when you’re pregnant you cannot digest pork and it rots in your stomach!” I just want to address some of the more common misconceptions.
· “You should not eat any seafood when you’re pregnant.” – On the contrary, seafood can be a healthy source of lean protein and iron and it is the only unfortified source of DHA, an omega-3 fatty acid that is essential for fetal brain development. You just don’t want to overdo it because seafood can contain mercury, a heavy metal that can build up in your blood. The general recommendation is to avoid fish that are high in mercury and aim for about 12 ounces/week of safe seafood. I included my recipe for pasta sauce with sardines at the bottom of this post.
· “You’ll have to cut coffee cold-turkey.” – Not if you don’t want to. The recommendation is to stay under 300 mg of caffeine a day, so a small cup of Joe can healthfully fit in to your diet. Worth noting – a Grande brewed coffee at Starbucks has 330 mg of caffeine vs. 190 mg in 16 oz brewed of most generic brands.
· “Ginger ale has no caffeine so drink as much as you want.” – It still has calories/added sugar and no nutritional benefits. If you are having morning sickness and it’s a choice between ginger ale and puking? Drink the ginger ale. Otherwise? Go for something else most of the time.
· “You have to eat meat when you’re pregnant.” – Nope. It is the position of the Academy of Nutrition and Dietetics that “Well-planned vegetarian diets are appropriate for individuals during all stages of the life cycle, including pregnancy [and] lactation.” You can easily meet your increased protein needs without turning to animal proteins. Vegans will need supplemental vitamin B-12 and anyone who doesn’t eat seafood should take a fish oil supplement. Vegetarians who are uncomfortable with the supplement should take care to consume walnuts, flax seeds, and chia seeds – but be aware that the conversion rate of ALA to DHA is estimated at only about 10%.
· “You are ‘eating for two’ now.” – Sadly, no. In the first trimester you don’t need any more calories than you did before you were pregnant. You only need about 340 additional kcal/day in the second trimester and 450 additional kcal/day in the third trimester. Your nutrient needs increase during pregnancy so if anything you have less wiggle room for junk food, not more.

The Diet “Traffic Light” for a Healthy Pregnancy
Recent studies have shown that presenting nutrition guidelines in a “traffic light” form can make them easier to digest, so to speak, so that is one of the ways I present information to my patients and the way and I will do it here.

Many of your vitamin and mineral needs increase during pregnancy – particularly calcium, folate, and iron – and it is important that you eat the foods that will meet those increased needs. That said, soon it will be summer and pregnant women tend to run hot, it will probably be pretty important for you to eat a bowl of ice cream too! I certainly don’t eat a perfect diet, and I don’t expect you to either. I tell my patients that “junk” (aka foods that make you happy but don’t provide any protein, vitamins, or minerals) is ok once or twice a week as long as they make sure they meet their needs first.
Stop: Do not consume these foods when you are pregnant
- Fish that are high in mercury: shark, swordfish, king mackerel, and tilefish
- Cold cuts/sandwich meat/deli meat that are served cold – these products have an increased risk of carrying a type of bacteria that grows at refrigerator-temperatures and should only be consumed steaming hot
- Raw or undercooked meat and poultry such as a medium-rare burger or steak tartare
- Raw or undercooked eggs such as soft-boiled eggs, sunny side up eggs, or hollandaise sauce
- Raw or undercooked fish, like sushi or lox
- Raw sprouts
- Raw or unpasteurized milk, unpasteurized cider or juices
- Dairy products made from raw or unpasteurized milk – many cheeses sold in America, including blues and Bries, have been pasteurized and are fine to have
- Alcoholic beverages; such as beer, wine, or spirits
- Any herbal supplements or teas that you have not checked with your healthcare provider
I don’t expect pregnant women to live in a bubble. There is inherent risk in leading a normal life. Riding in a car can be risky, but also fairly unavoidable. Ultimately you will have to weigh the costs/benefits of your choices yourself. My list of favorite foods is topped by coffee, diet soda, and soft-boiled eggs; perhaps when I’m pregnant I’ll decide the risk of me stabbing my husband in the face outweighs the risk of salmonella.
Caution: Limit these foods to once or twice per week
- Coffee and tea – you want to stay under 300 mg of caffeine/day
- Soda and other sweetened beverages
- Diet soda and other beverages with nonnutritive sweeteners – fake sugars are fine in moderation. The FDA has approved aspartame, acesulfame potassium, sucralose, saccharin, and neotame for general use. The American Medical Association advises avoiding saccharin due to possible slow fetal clearance.
- 100% fruit juice – consume no more than 8 oz of juice per day
- Albacore tuna and Atlantic salmon – consume no more than 6 oz/week of these “medium-mercury” sources
- Fried foods
- Refined grains like white bread and “sugar cereals”
- Empty calories; things like chips, fries, candy, baked goods, and bacon

Go: Eat these foods every day
- Low-fat or fat-free milk, yogurt, cottage cheese, and cheese, and/or calcium-fortified soy milk – at least three servings a day
- Fruit: fresh, frozen, dried, or canned in juice or water – at least two servings a day
- Vegetables: fresh or frozen – at least three servings a day; aim for one dark green veggie every day
- Whole grains such as bread, cereal, rice, pasta, oats, popcorn, and fortified cereals – you and your baby require at least 175 grams of carbohydrate per day
- Lean meat, low-mercury seafood, eggs, nuts, beans and legumes, and/or tofu
- Water

Finally, regular exercise is recommended for most pregnant women. If you are having a normal, healthy pregnancy – i.e. no bleeding, no bedrest, no insufficient cervical cerclage, and you’ve been cleared by your doctor – you should aim for at least 30 minutes of physical activity on most days of the week. Exercise can help reduce stress and constipation, lead to better sleep, and allow you to eat what you need to eat without excess weight gain. Don’t lie on your stomach or lie on your back after the 1st trimester. Don’t do anything where you might fall on or hit your stomach. Walking, swimming, yoga, supervised strength training, and use of the elliptical, treadmill, and stationary bike are all encouraged.
A Recipe! Sardine Mushroom Tomato Pasta Sauce
Sardines are one of the most concentrated sources of the omega-3 fatty acids EPA and DHA. These fantastic fishes also a good source of calcium and B-12. I find them to be a little scary straight from the can, this sauce is much less threatening.
Servings: 4
Prep Time: <5 minutes
Cook Time: 20-25
Ingredients
- 2 tsp olive oil
- 1 Tbsp butter
- (2) pints sliced, white mushrooms
- pinch salt
- (2) 3.75 ounce cans water-packed sardines, drained
- 2 cups of your favorite tomato sauce
Instructions
- Melt 1 tsp oil and 1/2 Tbsp butter in a large sauté pan over medium-high heat.
- Add mushrooms and salt to pan. Cook mushrooms, stirring regularly, for 10-15 minutes or until caramelized. Mushrooms should be reduced in size by about half and have developed a deeper brown color and amazing scent.
- Remove mushrooms from pan and reduce heat to medium.
- Melt remaining 1 tsp of oil and 1/2 Tbsp of butter (in the same pan you used for the mushrooms).
- Add sardines to pan and cook 3 minutes. Use the edge of a wooden spoon or spatula to break up the sardines into a paste.
- Reduce heat to low and return mushrooms to pan. Add tomato sauce, stirring carefully to combine. Cook another 2-4 minutes until the sauce has been fully heated through.
- Serve on top of whole-wheat pasta.

Sources
- Kaiser L, Allen LH. Position of the American Dietetic Association: nutrition and lifestyle for a healthy pregnancy outcome. Journal of the Am Dietetic Assoc. 2008; 108: 553-561.
- Academy of Nutrition and Dietetics. Academy of Nutrition and Dietetics Evidence Analysis Library. Accessed March 27, 2014.
- Academy of Nutrition and Dietetics. Nutrition Care Manual. http://nutritioncaremanual.org. Accessed March 28, 2014.

Emily Wax, RD, is a clinical Dietitian at a hospital in Brooklyn, NY, working primarily with prenatal patients in the outpatient Women’s Health Clinic. She worked as a teacher in East New York before returning to school for a 2nd degree, and she is thrilled to be back in NYC. She blogs sporadically at Eating Chalk about her life as a Registered Dietitian with a realistic diet.

Shannon says
This is a great roundup of pregnancy nutrition info all in one place! Thank you for sharing. I especially appreciate the point you made about vegetarian diets. A well-planned vegetarian diet is perfectly healthy for everyone, and more importantly, it’s just as important for meat-eaters to plan their own diets as it is for vegetarians.
emily says
Thanks, Shannon! Your point about everyone needing to plan ahead is a good one.
Livi says
This is so interesting! Definitely saving it away for my future needs!
Bridget says
Great info!! Emily or Kath – I would love to read more info about breastfeeding nutrition. I feel like I have a harder time feeling “full” while breastfeeding than I ever did while pregnant. I know that I need more calories and I often feel like no matter how well I try to eat I’m hungry soon after meals and snacks. Then there’s the whole lack of sleep and carb/sugar cravings.
emily says
There is clearly a lot more to this topic, but – are you getting enough water? Dehydration is common in breastfeeding women and that cannot definitely cause feelings of ravenous hunger. The baseline recommendation is 12 (8oz) glasses of caffeine-free fluids per day.
emily says
cannot = can, jeez!
jenn from much to my delight says
Terrific post! Thanks for so much important info.
Allison says
Very interesting and good to know you mustn’t live in a bubble while pregnant. Most of the recommendations didn’t surprise me other than the one on 100% fruit juice, why is there the recommendation to consume no more than 8 oz of juice per day?
emily says
When we talk about fruit consumption we are really pushing whole fruit. The juice has lost its fiber – meaning it won’t give you as much satiety, won’t help with constipation, etc – and tends to be fairly concentrated in sugar and calories. And unfortunately when we process fruit into juice we end up losing nutrients – most juices have lower levels of vitamins and minerals than their original fruits did.
Laura@SneakersandSpatulas says
I’m curious about why raw sprouts are a no-no?
emily says
Food safety concerns. Raw sprouts are very susceptible to bacteria contamination. According to the FDA, raw sprouts have been the source of 30+ foodborne illness outbreaks since 1996, mostly salmonella and e. coli.
Leah says
Interesting post, but seems to fit more on your baby blog.
KathEats says
Nutrition topics are all KERF!
Leah says
I guess it’s a gray area, but it just seems like this type of nutrition information does not apply to most of your KERF readers (or yourself, for that matter). But someone who reads BERF is quite possibly looking for just this type of post.
KathEats says
I think we all know someone who is pregnant, plus this has been on my post request list for a long time. I’m happy to cover all topics. If this one doesn’t suit you then just skip it!
Cristina says
This is an awesome post with lots of useful info on one page.
I would like your thoughts on aspartame. My ob/gyn is totally against it and most other “fake”sugars. I’ve done lots of reading on the subject and I’ve come to the conclusion that just because the FDA deems it safe, doesn’t mean it is. I try to avoid it. Thanks for the post!
emily says
All of the studies from the 80s/90s that found nonnutritive sweeteners to be harmful have since been discredited, but a lot of people tend to have residual fear. I think more research would be beneficial, but every (peer reviewed, double-blind, etc) study done thus far has found aspartame to be safe in moderation. It is important to remember that new, unstudied products hit the market all the time – Stevia, for example, has not been approved for prenatal use yet.
Helen says
Well this was an interesting read. I don’t agree that fat free dairy is best, and was surprised to see bacon listed as an empty calorie food!
emily says
Well I didn’t say “bacon – the silent killer” but it is hardly a nutritional powerhouse. 2 slices of pork bacon contain an infinitesimal amount of iron versus the 1 mg in 4oz of pork chop.
vks says
What if you cook it in cast iron? And then make a BLT with spinach/kale instead of lettuce? On whole grain bread? I lived on BLTs during my first trimester. It was that or macaroni and cheese!
Natalie says
Bacon from pasture-raised pigs is actually very high in vitamins E and D.
Chelsea@TableForOne says
This is great advice! I get questions all the time from my sisters about the things they need to be doing in order to have a healthy pregnancy. These are things all women need to hear and want to know.
lauryn says
great post very informative, i will prob go back and read it again in the future!
Becky@TheSavedRunner says
I loved learning all of this information. Thank you for sharing. I am about to send this to my friend who is pregnant!
Jenn says
I’ve lost 4 babies to incompetent cervix and although your post is informative it really does glorify the healthy pregnancy and doesn’t call attention to the difficulties that some ladies face. I exercised regularly during my first pregnancy because I thought it was the thing to do (you know #fitpregnancy and all) and ended up delivering at 22 weeks because you have no idea your cervix is incompetent until after the fact. Getting pregnant and staying that way isn’t easy for some people and some of us would be willing to make a deal with the devil to have a baby. I’m facing 9 months of bedrest hoping that I’ll get my rainbow. I can assure you that gaining too much weight is really really really low on my priority list.
KathEats says
Jenn, I’m really, really sorry to hear that. Emily’s post is about basic nutrition and doesn’t cover high risk cases, which should be addressed by each individual’s doctor.
emily says
Jenn, I am so sorry about your losses. My sister-in-law had an incompetent cervix and her 4+ months of bed rest were very rough. (She recommends fellow bed resting mamas get an unlimited Netflix subscription!) The guidelines for high-risk pregnancies are indeed very different.
Danielle says
This is an interesting point. I lost my daughter Sofia at 23.5 weeks- no reason. However, it would be an interesting topic to discuss on BERF. I hope that l your pregnancies never end in loss kath, but it might be good to present the other side to pregnancy- some of the realities of loss.
KathEats says
I’m very sorry to hear that Danielle. My mom lost a baby in the middle of her second trimester, so while I was too young to remember, miscarriage has touched our family as well.
tonya says
As someone who at a young age miscarried twice (both boys) due to an incompetent cervic, I don’t think it’s fair to ask someone who has not suffered that kind of loss to write a post giving insight to our painful experience. Surely there are other blog resources for that discussion. Let this post be what it is and not demand that every single post meet our very personal and specific needs.
tonya says
Also I am terribly sorry about your loss. Again, I’ve lost two myself. It is a pain that you never really get over. My heart goes out to you. But my point was can you imagine the outrage and backlash kath would get for writing about loss and risky pregnancy when she was blessed to not have that experience? You see how upset people get over posts about salads LOL
Danielle says
I was more thinking she gets someone who had experienced a pregnancy loss to write it. Also, I just said it would be an interesting discussion and I wasn’t demanding or seeking a need for it. It’s more because pregnancy loss in general has such a stigma attached to it, I thought it could bring an open and healthy discussion. If laths mum ever felt that she could write about her experience I think it would be an honour to read it. As I said- it would be an interesting discussion.
Kat says
I would like to correct some of the items in your “stop” list. Cheeses that are aged more than 60 days (most cheeses sold in the US are aged…the only one that i have researched that is actually unsafe is queso fresca the mexican cheese) are totally safe for pregnancy, and the chance for getting listeria from raw fish, especially at a high quality sushi restaurant is very very low. There’s a lot out there to scare pregnant women, but really women have been eating whatever they want for centuries so it’s important to do research and decide what you’re comfortable with. This is my strategy at least, and I think more women get scared rather than do their own research.
Lori says
Women have been eating whatever they want for centiries, and have also been having miscarriages and delivering stillborn babies for centuries, too. With time comes reseach and this kind of info is just much more readily available today. While I agree that very high quality raw seafood is probably fine, that’s probably not what most people have access to. I’m not saying you said this, Kat, but I have heard women say that they are not going to give up lunch meat because the risk of listeria is so low and why should they live in a bubble, and I think that’s just sad. Is a turkey sandwich really worth the chance of a stillborn baby?
Steph says
I have a question about pregnancy weight gain. I am 14 weeks pregnant with my 3rd child. With my first two I gained 36 and then 49 lbs while pregnant. I had no problem losing all the weight afterwards within a 6 month time frame, without doing any diet (except being a 24-hr milk machine!) My question is, is it harmful to gain more than the recommended amount during pregnancy? Apart from the worry of not losing that extra fat after the baby is born, does the extra weight gain negatively affect the baby or mommy at all?
emily says
It really depends… the guidelines are general, not set in stone, and they are not going to be right for every person/pregnancy. Gaining weight in excess of what is right *for you* can lead to macrosomia – large for gestational age baby – which may make a vaginal birth dangerous/impossible, lead to excess postpartum weight retention, and increase the newborn’s risk for a variety of life-long medical conditions, etc. Excess weight gain is especially worrisome in cases of gestational diabetes because it may relate to poor glucose control.
Every pregnancy is different though. Your previous pregnancy gains (and childrens’ birth weights) tend to be a good indication of what to expect; I bet your Dr/RD will tell you to aim towards the upper end this time based on your past pregnancies.
Chelsea @ Designs on Dinner says
Great post! I did just read an article stating that sushi is fine to eat while pregnant as long as it is a low-mercury fish. Japanese women eat sushi as part of their regular diet, and it is not known to cause pregnancy complications there. Must be one of those “better safe than sorry” claims? Lots of great tips, though!
marie says
I feel your first paragraph under ‘common myths’ is somewhat harsh. I went through three pregnancies and always felt flattered that people were so happy for me and wanted to discuss my baby. We live in a society were talking to strangers on a train or in the market is becoming scarcer because people are so afraid of offending each other. Yes we’re sick and bloated and nauseous, but let’s find the joy in making connections with people.
emily says
Marie – fair point! I was being a little hyperbolic for human’s sake 🙂
emily says
*humor’s
Sarah says
I am really surprised that someone with a nutritional background would recommend diet soda. It is one of the worst things anyone, especially pregnant woman, could drink/eat.
KathEats says
She’s not necessarily recommending it but saying that it should be a caution food. There are many, many people who drink a lot of soda and this is part of the education for the general public.
emily says
Sarah, we will have to agree to disagree, but if you have research I’m unaware of that supports that I’d love to see it. ?– seriously, I feel like that sounded sarcastic but I’m being genuine
Sarah says
Helpful post!
One thing I’ve heard mixed things about is whether it’s fine to eat peanut butter. I would assume it was fine, but a mom friend of mine told me her daughter’s egg and peanut allergies were her fault, since she ate peanut butter during pregnancy…
What’s your opinion?
KathEats says
It’s fine! There’s nothing that I have heard against it. Someone correct me if I’m wrong, but I think the more things you stay away from the greater chance of allergies – at least when feeding kids. Peds used to tell parents to wait a few years on things like eggs and peanut butter but they found that kids were getting allergies less if they were introduced in the first year.
emily says
Kath is correct! And the most recent research on introducing highly allergenic foods like eggs and dairy says there’s no reason to delay beyond 4-6 months with other solids. In fact, according to the American Academy of Allergy, Asthma, and Immunology “delaying introduction to these foods mat increase your baby’s risk of developing allergies.”
Sorry to get off topic, I just found that interesting!
Christine says
Would this also apply to fruit? I had offered some strawberries to my friend and her daughter (6 months old) and she said her daughter was too young for strawberries and had to wait until after 1year. I had never heard of that, thanks!
Steph says
I have a question about weight gain. I am 14 weeks pregnant with my 3rd child. During my first pregnancies I gained 36 and then 49 lbs. I had no problem losing the weight within a 6 month period post-birth without dieting, but simply being a 24-hr milk machine! My question is, are there any harmful side effects of gaining more than the recommended amount during pregnancy? Does it hurt the baby or Mommy at all? As long as the weight comes off afterwards is it bad to gain 40+ lbs?
emily says
Steph – your question went through twice; I answered above 🙂
Laura says
I have been eating seafood (of any type) 1x per week since I was under the assumption that was the “safe” guideline. However, do you suggest to your clients that they can eat shrimp multiple times a week? If so, I would be happy to know this! Thanks!
CaitlinHTP says
This was such a great post and so well written! I really enjoyed it. Pinning now!
emily says
Thanks, Caitlin!
Christine says
Hi Emily!
Thank you for the great post, very informational! I’m 17 weeks pregnant with my first. Prior to my pregnancy I was watching my weight and counting calories. I was actually trying to lose some weight and was around 1200-1400 calories a day(with weight watchers). Is there a minimum amount of calories a pregnant woman should consume per day? I am 5’8 and started at 155 lbs…I am now at 165lbs.
I know most people have told me (including my doctor) to just eat when I’m hungry, listen to my body and make healthy choices…but I’m still in that calorie counting mind set. Is there a number I can focus on? Is adding 350 cal to my prior 1400 cal a day diet enough? Thank you!
emily says
I’m not comfortable giving you a specific number but generally speaking you add 340 calories in the second trimester and 450 calories in the third trimester on top of the calories you needed before you got pregnant. That said, the calories you needed depend on many factors: weight, height, BMI, age, activity level…
If you feel like you miss counting something and the tracking gives you peace of mind, I would recommend “counting/tracking” food groups; check in each day to make sure you ate enough dairy, vegetables, etc
emily says
As long as you stay away from the high mercury options – shark, swordfish, tilefish, and king mackerel – multiple times a week is completely safe, the general guideline is not to exceed 12 oz total per week. Shrimp are not high in mercury, though sadly they are not that high in omega-3s either.
emily says
Crap! Kath, I’m a commenting disaster. This was supposed to be in response to Laura’s question.
Ashley @ Coffee Cake and Cardio says
As a plus size pregnant woman, the recommended weight gain based on BMI is incredibly frustrating to me. In my opinion, it is near impossible to only gain 11-20 pounds when as the first graphic shows most will gain 30 pounds of baby/pregnancy additions before body fat even comes into play. I have found that in order to stay in the recommend weight gain range I essentially have to lose weight and only gain baby. It’s really disgusting if you ask me.
I think that our society needs to do a better job of educating “obese” pregnant women instead of telling them to only gain x number of pounds and making them feel like less of a person because they’re heavy. I am not perfect by any means. but I am striving to eat as healthy as possible and I work out quite a bit. Even so, I have already gained more than I should at this point in my pregnancy (25 weeks). I can honest to God say that the only way I could slow down my gain is by dieting, which is a no-no according to 90% of doctors. I say 90% because I have heard of doctors telling “obese” women to reduce calories (aka diet) while pregnant.
I applaud “obese” women who stay under their recommended weight gain total. What I’ve learned is that every woman is different and in a lot of ways the gain during pregnancy is out of our control. All we really can control is what we eat and how we move. If we gain regardless, then we gain. Women shouldn’t be looked down upon because their bodies decide to add more while growing a human.
End rant 🙂
KathEats says
Totally agree Ashley! I think the numbers are just set for guidelines, but everyone is so different that it’s really up to your own doctor and you to figure out what is best for your body.
emily says
What Kath said! And I’m sorry if you feel like people responsible for your prenatal care have tried to fit you into guidelines that were too narrow, when I am working with patients one-on-one I definitely deal with them as an individual.
Resh says
Hey Emily! This is so helpful – thanks! Would love to hear more thoughts on the alcohol. As you likely know, some doctors are more liberal with the suggestion of stopping completely. Some agree with you that alcoholic beverages should not be consumed at all. I’m not pregnant, but have noticed that my friends spam the spectrum and I try not to ask anyone anything because it seems like it’s a touchy subject!
emily says
I encourage my patients to abstain the entire pregnancy. We honestly don’t have the best research on the effects of minimal amounts of alcohol on the fetus because the types of studies you would have to design to test this would be unethical. We know that “too much” alcohol can have devastating effects and we don’t currently have research that can support a safe amount. That said – I don’t think it’s the end of the world if you taste a new beer a friend is drinking or get married mid-pregnancy and have a champagne toast.
Lori says
I have read that too much soy during pregancy can affect the proper development of a baby boy’s genitals, specifically the location of the urethra. Should soy products really be listed in the green category?
emily says
There has been a lot of conflicting research regarding soy and cancer risk, males, etc. At this point the recommendation is to eat more-processed soy – things like soy lecithin in Luna Bars – in moderation but that whole soy – for example, tofu – can be beneficial.
Kara says
Interesting read~ But I cant help but wonder if this is leading to a Bigger Announcement!! 🙂
KathEats says
Ha nope!
Ali says
I am in my first trimester, and nearly all forms of protein make me extremely nauseous. I can stomach dairy (three cheers for greek yogurt), but my old favourites like beans (in all forms – including hummus), meat, fish, nuts, eggs, and even quinoa make me incredibly nauseous….even just thinking about them now makes my stomach churn. I am trusting that my appetite will come back after the first trimester, but I am so stressed about the protein component at this stage. Any suggestions?
KathEats says
Ali you make me nauseous just thinking about how sick I felt in my first trimester thinking about those foods!!! For me things got a lot better at 14/15 weeks and I could eat almost everything again. Hoping it’s the same for you!
Emilie says
pressed cottage cheese! 24 grams of protein per serving.
emily says
My number one suggestion? Stop stressing! I tell my clients that there is the “healthy pregnancy diet” and then there’s the “first trimester diet;” you just want to do the best you can, which does not include forcing yourself to eat things that will make you puke. We usually see a major drop in morning sickness symptoms and food aversions around 14 weeks.
The dairy is awesome; if you are doing three servings a day that is 36 grams of protein right there. Other ideas include – cottage cheese (13 grams pro per 1/2 cup), tofu (20 grams pro per half cup), chia seeds (3 grams pro per Tbsp), and pumpkin and sunflower seeds (8.5 and 5.5 grams pro per oz). And don’t forget that you’re getting a bit of protein from your grains as well; and if you can stomach whole grains instead of white/refined products they will have a little bit more protein and fiber.
If you’re doing oatmeal you can stir in a whole egg while it cooks and if you can do smoothies you might be able to stomach adding some silken tofu or a scoop of peanut butter to increase the protein (and definitely make sure to make your smoothies with yogurt and milk versus water or juice).
I hope that helps!
Ali says
Great suggestions – thanks! I read the ‘ 70 grams of protein’ recommendation and stress, but it is true that at this point it probably does not matter as much. Thanks for the egg-in-oatmeal suggestion, and the tip about adding more protein to smoothies. Anything fruit-based is awesome right now, so I’ll give that a try. Thanks!
Melissa says
What a fantastic and informative post!
For someone who is looking to get pregnant in the next year or two, I am happy to take in such valuable information and share with my friends who are in the same boat as me.
Kate says
Great post – thank you. I am 15 weeks pregnant. My question is: if you aren’t supposed to add any extra calories in the first trimester, then why was I so hungry all the time? My appetite nearly doubled, to the point where sometimes I woke up in the middle of the night starving. I’m sure it wasn’t just my imagination. Curious to hear why that might be….
emily says
Thanks, Kate! The increase in hunger is believed to be due to hormonal changes.
Emilie says
I live in Canada, and while most of the recommendations you mentioned are the same, during my most recent pregnancy (last year) my midwife (they are as plentiful and qualified as OB’s up here) was fine with me consuming sushi in moderation, as well as raw eggs on occasion. I realize the POTENTIAL risks for these foods, however, if these foods are eaten as a rare treat I see no reason to limit them. As another commenter mentioned, women eat these foods daily in traditional food cultures today and have no ill effects. Of course, its all about quality of sources.
Resh says
Hey Emily! This is so helpful – thanks! Would love to hear more thoughts on the alcohol. As you likely know, some doctors are more liberal with the suggestion of stopping completely. Some agree with you that alcoholic beverages should not be consumed at all. I’m not pregnant, but have noticed that my friends spam the spectrum and I try not to ask anyone anything because it seems like it’s a touchy subject!
Rebekah says
Great post! I’m 26 weeks along with my second baby, and it’s nice to get a refresher of all the rules and guidelines. It didn’t even occur to me that hollandaise sauce was unsafe! I know I had it once on top of steak during this pregnancy. Now I know! Thanks for all the great info!